Mental health care is complex — and so is the medication that supports it. Behind every administration lies a careful balance of trust, timing, and safety, which clinicians must constantly navigate. Ensuring treatment is delivered safely is already a challenge, but for patients treated under the Mental Health Act (MHA), every prescription carries an additional layer of legal and ethical responsibility.
Historically, Oxford Health NHS Foundation Trust relied on paper-based consent forms to manage this process. T2 forms were completed by the ward responsible clinician when patients could consent to treatment; T3 forms required a second opinion doctor when patients lacked capacity or refused treatment. But paper forms introduced risk and inefficiency: they could be misplaced, illegible, or outdated, which complicated cross-checking, delayed treatment, and increased the potential for errors.
The challenge of paper-based consent in NHS mental health care
When Oxford Health first implemented electronic prescribing and medication administration (ePMA), multiple processes ran in parallel, creating additional complexity. The baseline audit revealed significant gaps in compliance, particularly in the availability of forms on wards and the completion of Section 62 documentation.
Digitisation emerged as a critical requirement during supplier engagement in the tender phase. This represented a first-of-its-kind request for our ePMA solution, Better Meds, highlighting the Trust’s commitment to safety, efficiency, and compliance.
Lex Moon, Digital Medicines Clinical Lead at Oxford Health and the lead on the ePMA project, shared with us just how necessary the change was, noting that the existing barriers made delivery of care more complicated, inaccurate, and potentially unsafe.
Designing a digital consent solution for MHA requirements
“Working with Oxford Health on the complex topic of T2/T3 forms was facilitated by their dedication and collaborative approach, translating requirements into a usable solution for all our customers.”
— Christine Wadsworth, Better UK Clinical Lead
From the outset, Oxford Health worked closely with Better Meds to ensure the solution was both clinician-friendly and fully compliant. Key stakeholders — including the MHA office, senior clinicians, pharmacy, nursing teams, and external bodies such as the CQC — were involved in designing the system functionality. Mock forms and detailed workshops helped clarify requirements and their underlying rationale.
Feedback from other trusts ensured the solution was broadly applicable, not just trust-specific. During this design phase, paper T2/T3 forms were retained as an interim solution, maintaining continuity while staff familiarised themselves with the new digital workflow.
Implementing digital consent across the NHS Trust
Once the initial release of the consent-to-treatment functionality was ready, Oxford Health led User Acceptance Testing, incorporating feedback from internal teams, other trusts, and the CQC. Better Meds updated the system iteratively, ensuring it met both clinical and regulatory expectations.
The functionality was first piloted on a single ward, providing valuable real-world insights that informed refinements. Following this, a structured two-week rollout deployed the system across all 25 mental health wards, ensuring a smooth and consistent transition.
“This functionality ensures proactive MHA compliance for mental disorder treatment. Digitisation prevents misinterpretation of handwritten documents, reduces the risk of unauthorised medication prescribing, and promotes efficiency in MHA processes.”
— Emma Bradley, MHA Office Manager, Oxford Health NHS Foundation Trust
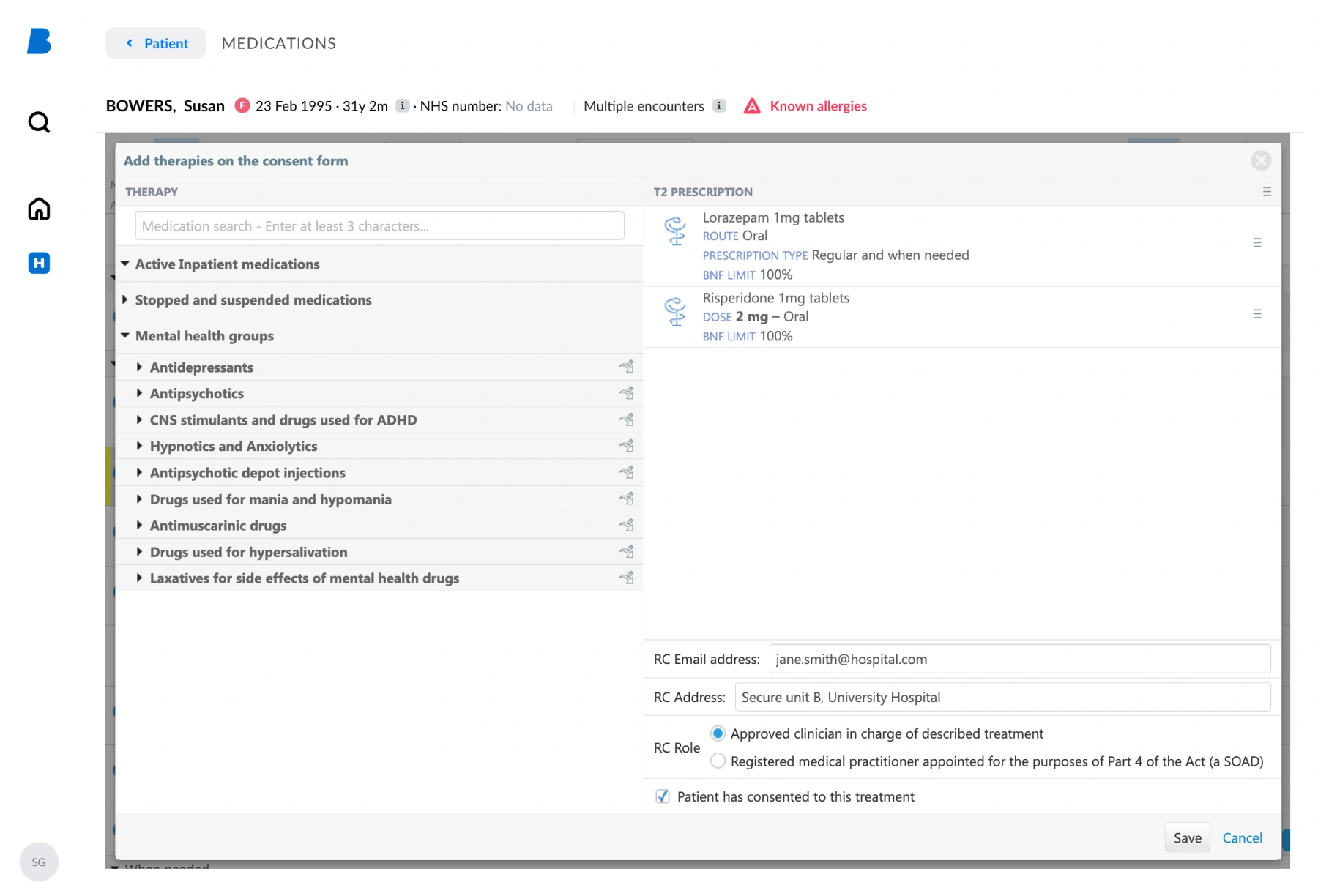
How digital consent forms work in Better Meds
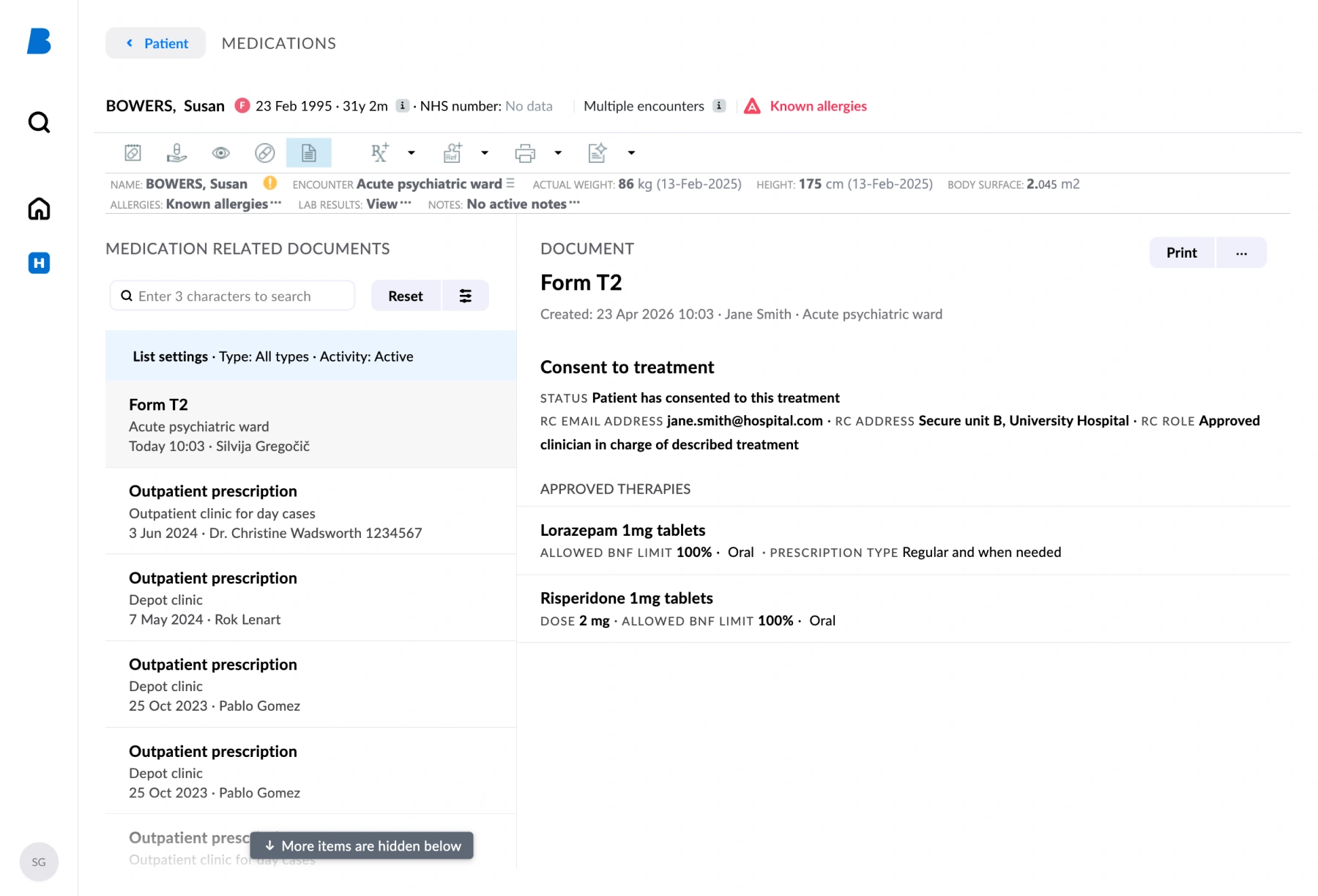
Now that their digitalisation is complete, T2 forms are created within the Better Meds system by the responsible clinician. T3 forms, once received from the CQC, are transcribed into the system by the responsible clinician or a nominated junior doctor. Digital consent forms are now directly linked to prescriptions, providing real-time decision support directly at the point of prescribing. High-level override warnings flag prescribing outside authorised treatment, and the relevant T2 or T3 form is clearly identified on the MAR chart. Staff can complete audits, reporting, and essential checks more efficiently and accurately, directly reducing clinical risk.
Training and support were carefully designed to address potential digital inequalities:
- E-learning modules for existing and new staff.
- Short instructional videos (<3 mins) covering T2/T3 creation and viewing.
- Face-to-face support for those who preferred hands-on learning.
At go-live, the digital medicines team provided real-time support on wards, boosting confidence and adoption.
The impact on MHA compliance, safety, and efficiency
Early audits post-rollout show improved compliance, stronger Section 58 adherence, and safer medicine management. Staff report less anxiety, faster prescribing, and clearer documentation. Importantly, digitisation has freed time for patient care while reducing paper use.
“The T2/T3 functionality allows efficient transcribing of these forms and ensures all prescribed medications are covered for MHA compliance. Once created, forms can be quickly edited to reflect any changes to the treatment plan.”
— Mark Hancock, CCIO & Psychiatrist, Oxford Health NHS Foundation Trust
“As a new pharmacist in Mental Health, I have found the T2/T3 on Better Meds extremely useful as a quick reference tool to ensure MHA compliance for patients. It is extremely exciting that this kind of thing can be incorporated into digital drug charts.”
— Rachel Comer, Pharmacist, Oxford Health NHS Foundation Trust
What’s next for digital consent in mental health care
The journey continues: digitised Section 62 forms are planned to be piloted and rolled out in the near future along with CTO11 and CTO12 outpatient equivalent consent forms. These will be tested by the community mental health teams once available.
Designed to be fully compliant yet widely applicable, this first-of-its-kind system can be adopted by any trust caring for patients detained under the MHA. The project has gained national recognition by being shortlisted for major digital health awards (HSJ Digital Award and HTN Award), celebrating innovation, impact, and collaboration, and international acclaim, as Lex Moon won the College of Mental Health Pharmacy’s Oral Pharmacy Practice Presentation Award for working on this initiative. Recently, Oxford Health has also been recognised as the Regional Champion in the Digital Innovation category of the NHS Excellence Awards, another testament to the value of digital medicines innovation in mental health.
As Oxford Health demonstrates, digital transformation isn’t a one-off project, but a continuous journey of evolution, where technology and people come together to safeguard care, empower clinicians, and improve outcomes.
Discover how Better Meds can support your team, medication processes, and patient safety.